ITC Compounding Pharmacy was established in 1994. Our mission is to provide our customers with the highest quality compounded medications. We use only the finest quality of ingredients in their purest form. Our state-of-the art equipment, quality assurance, customer service, and experienced staff, make us a premier source for customized medications. At ITC, all medications are made for our patients specifically from doctor’s orders to ensure correct dosage forms and delivery methods. As a compounding-only pharmacy, we work very closely with our providers to develop treatment options and protocols that provide optimal results. We listen to you and will work with you and your healthcare provider to address your specific needs to achieve optimal results.
Welcome to ITC Compounding Pharmacy

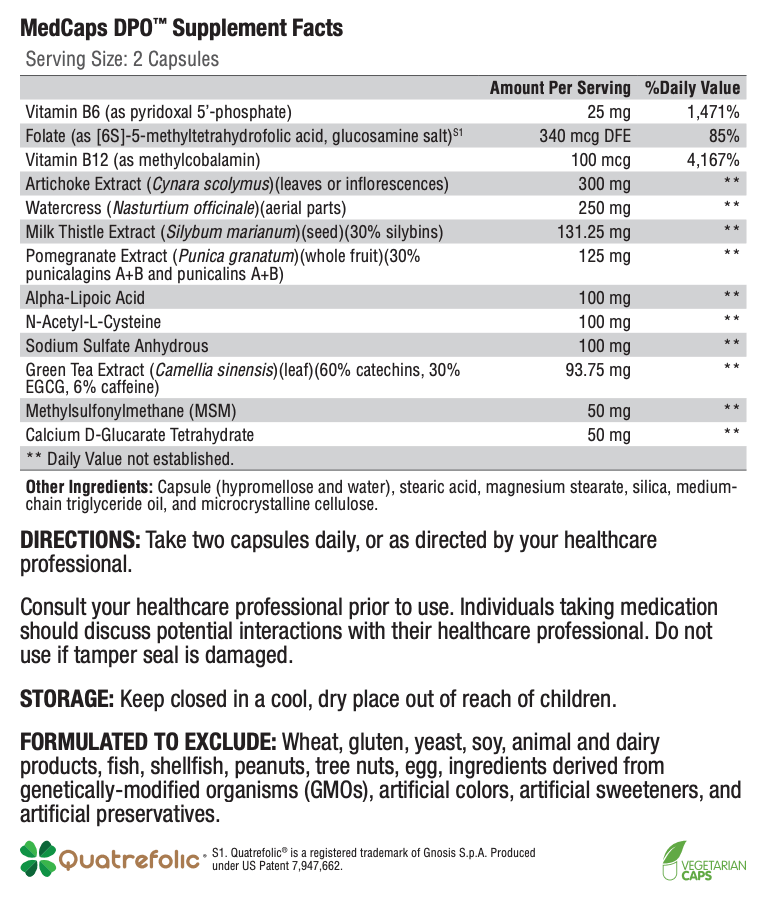
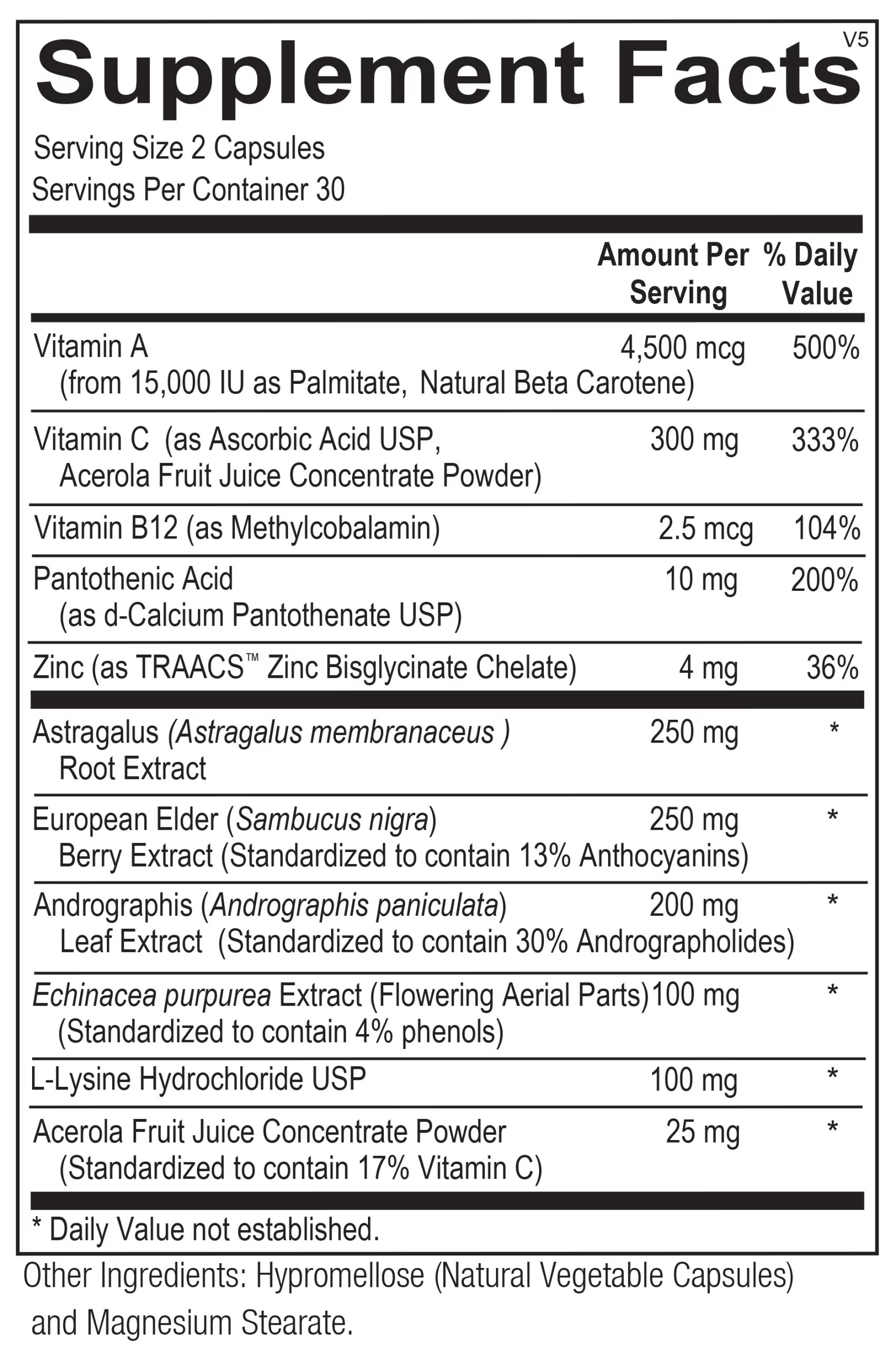
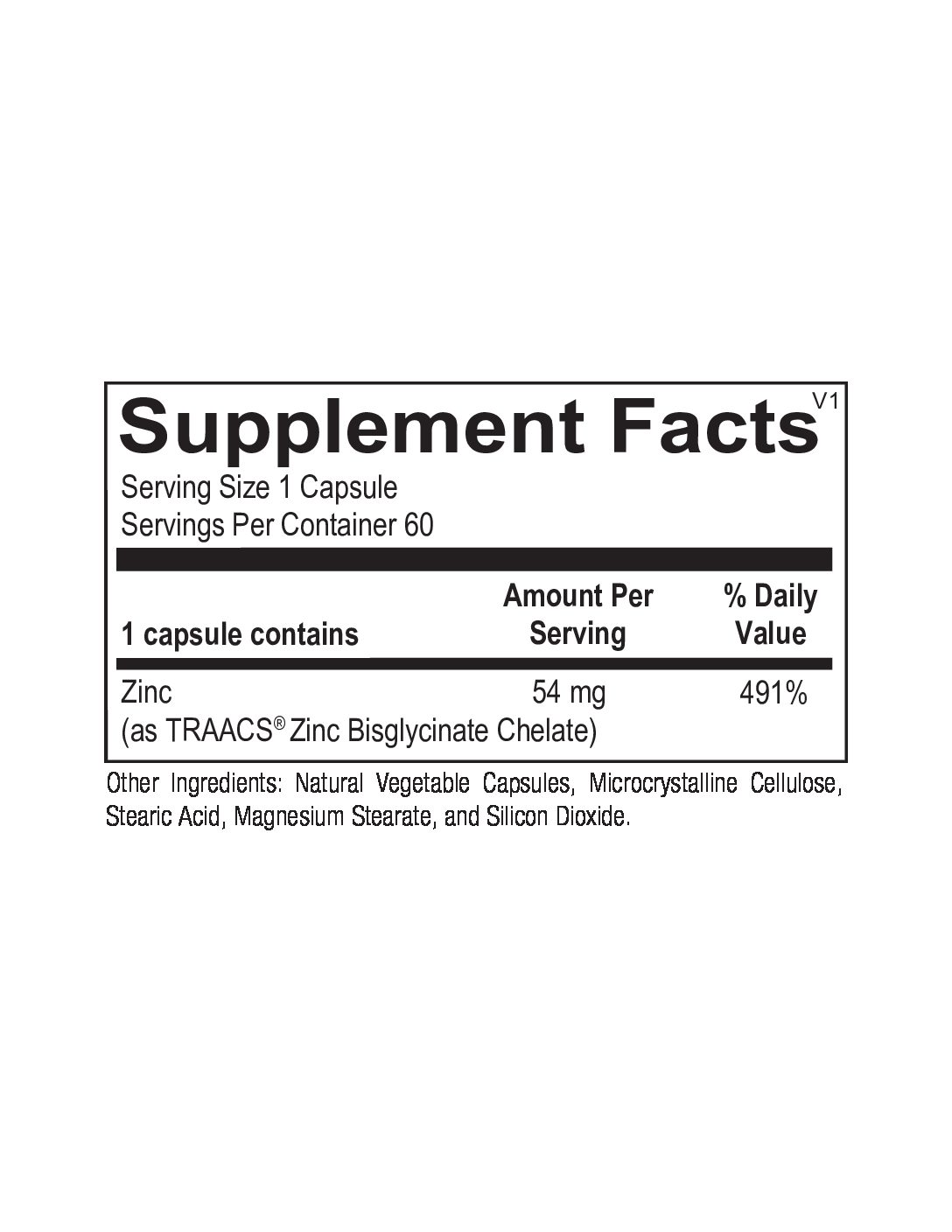
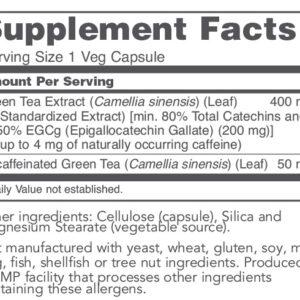
Offering the very best nutritional supplements to help you care for you and your family.
ITC Pharmacy is committed to compounding the highest quality of customized medications.
HORMONE THERAPY
Learn about customized hormones and other options to balance your system.
PAIN MANAGEMENT
We can offer alternative options to traditional treatment for pain.
SKIN CARE
ITC can compound individualized formulations for various skin conditions.
VETERINARY MEDICATIONS
Animals are individual and unique. ITC provides solutions to your medication challenges.